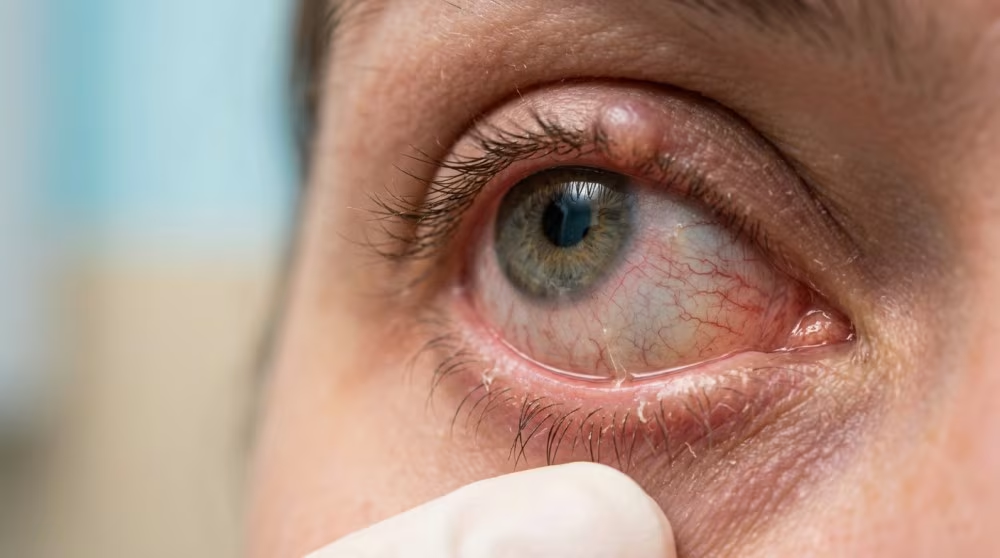
If you have ever felt burning, irritation, or fluctuating vision – especially when reading or working on a computer – you may have experienced dry eye disease. As an ophthalmologist, this is one of the most common conditions I see in clinic. Many patients assume dry eye is a minor annoyance, but in reality it can significantly affect comfort, vision, and quality of life. The good news is that we understand the condition much better today than we did even a decade ago, and there are many effective treatment options.
What Is Dry Eye Disease?
Dry eye disease occurs when the surface of the eye does not have a healthy, stable tear film. The tear film is a very thin layer of fluid that coats the eye every time we blink. It keeps the surface smooth, nourished, and protected.
The tear film actually has three important components:
- Oil layer – prevents tears from evaporating too quickly
- Water layer – provides moisture and nutrients
- Mucus layer – helps tears spread evenly across the eye
If any part of this system stops working well, the tear film becomes unstable. When that happens, the surface of the eye dries out and becomes irritated.
In simple terms, dry eye happens because either:
- You don’t make enough tears, or
- Your tears evaporate too quickly.
Most patients actually have a combination of both.
Symptoms of Dry Eye

One of the interesting things about dry eye disease is that symptoms can vary widely. Some patients have significant discomfort, while others mainly notice vision fluctuations.
Common symptoms include:
- Burning or stinging
- A gritty or sandy feeling
- Redness
- Blurry or fluctuating vision
- Light sensitivity
- Eye fatigue
- Excess tearing
- Difficulty with reading or computer work
The symptom of excess tearing surprises many patients. It seems counterintuitive, but when the eye becomes irritated from dryness, it can reflexively produce a surge of watery tears. Unfortunately, these tears do not stay on the eye very well and do not solve the underlying problem.
Symptoms often worsen in certain situations:
- Prolonged screen use
- Reading
- Air conditioning or heating
- Windy environments
- Airplane travel
- Contact lens wear
Patients frequently tell me their eyes feel worse later in the day, after hours of visual tasks.
Different Types of Dry Eye Disease
Dry eye is not a single condition. In ophthalmology we usually divide it into two major categories.
1. Aqueous Deficient Dry Eye
This occurs when the lacrimal glands do not produce enough tears.
Causes may include:
- Aging
- Certain medications (antihistamines, antidepressants, blood pressure medicines)
- Autoimmune conditions such as Sjögren’s syndrome
- Previous eye surgery
- Hormonal changes
In this form of dry eye, the eye simply does not have enough tear volume to maintain a healthy surface.
2. Evaporative Dry Eye
This is actually the most common form of dry eye that I see in clinic.
In this type, tears are produced normally, but they evaporate too quickly. The most common cause is dysfunction of the oil-producing glands in the eyelids, called the meibomian glands.
When these glands become clogged or inflamed, the tear film loses its protective oil layer. Without that oil layer, tears evaporate rapidly, leaving the eye dry and irritated.
Factors that contribute to this include:
- Aging
- Rosacea
- Long hours of screen use
- Incomplete blinking
- Contact lens wear
In my experience, most patients have a mixed form of dry eye that includes both evaporative and aqueous deficiency.
Why Dry Eye Is So Common Today

Dry eye disease has become increasingly common over the past several decades. One major reason is modern visual behavior.
When we look at screens -phones, tablets, computers – we tend to blink less frequently. Studies show blink rates can drop by nearly half during computer use.
Less blinking means:
- The tear film is not refreshed
- Oil glands are not stimulated properly
- Tears evaporate more quickly
As a result, many patients develop symptoms after long days at work.
Environmental factors also play a role. Indoor air conditioning, heating, and low humidity can all worsen dryness.
How We Treat Dry Eye Disease
Treatment for dry eye works best when it addresses the underlying cause, rather than just masking symptoms.
I usually think of treatment in several layers.
Artificial Tears
For many patients, the first step is lubricating eye drops.
These drops supplement the natural tear film and improve comfort. They are available over the counter and can be used several times a day.
In general, I recommend preservative-free artificial tears, especially if patients are using drops frequently.
While artificial tears can help symptoms, they do not usually treat the underlying inflammation driving dry eye disease.
Warm Compresses
For patients with evaporative dry eye, improving the function of the eyelid oil glands is essential.
Warm compresses help melt thickened oils in the glands and allow them to flow more normally.
Patients often benefit from:
- Warm compresses for 5–10 minutes daily
- Gentle lid massage
Consistency is important. These therapies work best when done regularly.
Anti-Inflammatory Treatments
We now know that inflammation plays a central role in dry eye disease. For patients with persistent symptoms, prescription medications may help reduce inflammation on the eye surface. In the short term, steroid drops are an effective treatment, but may have side effects if used as a long-term treatment.
Other classes of anti-inflammatory medications do not provide instant relief. Instead, they work gradually by improving the health of the tear-producing tissues.
Patients typically notice improvement over several weeks to months.
Punctal Plugs
For patients who do not produce enough tears, we can sometimes place punctal plugs.
These are tiny devices inserted into the tear drainage ducts of the eyelids. By partially blocking tear drainage, they allow tears to remain on the eye longer.
The procedure is quick and performed in the clinic.
Antibiotic Treatments
Some forms of dry eye syndrome are caused by bacteria. If I suspect that bacteria are worsening dry eye disease, I will sometimes recommend oral antibiotics. Lid scrubs can also reduce the bacteria on the eyelids.
Advanced Therapies
In more significant cases, additional treatments may help, such as:
- Thermal treatments to open clogged oil glands
- Intense pulsed light (IPL) therapy
- Prescription medications that stimulate tear production
- Autologous serum tears in severe disease
Fortunately, most patients improve with a combination of simpler treatments and lifestyle adjustments.
Practical Tips I Often Share With Patients

Beyond medical treatment, small changes can make a meaningful difference:
- Blink consciously during screen use.
- Stay well hydrated.
- Consider wraparound glasses in windy conditions.
For patients who spend long hours at a computer, these simple strategies can significantly reduce symptoms.
The Bottom Line
Dry eye disease is extremely common, but it is also very treatable. The key is recognizing that dry eye is usually a chronic condition that requires ongoing management.
There are many factors that affect dry eye. The most common on environment triggers, allergies, inflammatory disease, blepharitis, systemic medications, and hormonal changes. Because there are many contributors to dry eye, each patient may require a different combination of treatments to address their specific disease. My goal is to identify the main causes and address them. Sometimes these are obvious in the beginning, but sometime it may take trial and error with many office visits.
The bottom line is that we are committed to making you see and feel better. We will use our expertise along with many different possible treatment modalities to treat your disease.